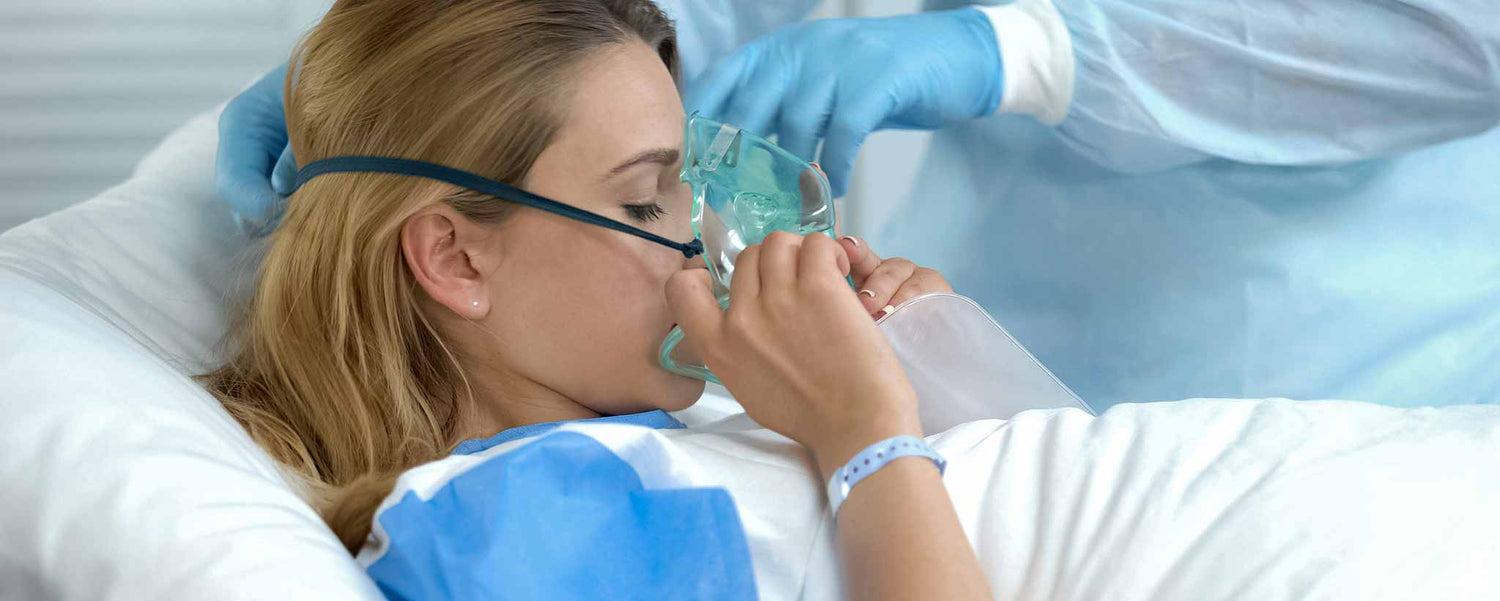
With many improvements to lung transplant surgery since the 1980s, post-op requires a daily cocktail of immunosuppressive drugs and antibiotics.
Reasons For Lung Transplants
November is COPD and Lung Cancer Awareness Month
As a last resort, single- or double-lung transplants, as well as heart-lung and partial-lung transplants are possible. There aren’t enough donor lungs for everyone who needs them.
Transplant centers prioritize according to local criteria along with some generally accepted national guidelines. For example, a history of noncompliance with medical instruction or multiple concurrent diseases can classify a patient as a poor pulmonary transplant recipient.
In June 2020, a woman in her 20s with irreversible lung damage from COVID-19 was the first in the United States to receive a double-lung transplant. Organ transplants may become more common in severe cases of COVID-19. —Medscape
Anatomy posters and models simplify explanation of medical procedures. There have been many improvements to lung transplant surgery since the 1980s. This includes powerful anti-rejection drugs and bloodless medical management techniques when warranted. As of 2005, the most common reasons for lung transplantation in the United States were:
- 27% chronic obstructive pulmonary disease (COPD), including emphysema
- 16% idiopathic pulmonary fibrosis
- 14% cystic fibrosis
- 12% idiopathic (formerly known as “primary”) pulmonary hypertension
- 5% alpha 1-antitrypsin deficiency
- 2% replacing previously transplanted lungs that have since failed
- 24% other causes, including bronchiectasis and sarcoidosis
Increasingly, lung transplantation is an option among severe COVID-19 patients. A challenge that researchers are discovering is an unexpected disease pattern in COVID-19 lungs: The virus invades the cells that line blood vessels, called endothelial cells, and this causes blood clots—9 times more than typical influenza. These clots can lead to thrombosis or strokes.
It is now clear that COVID-19 damages more than your lungs. In a medical review of patients around the world, coronavirus compromises the kidneys, liver, heart, brain and nervous system, skin, and gastrointestinal tract. Hospitals cannot just staff pulmonologists during the pandemic. COVID-19 is a “multi-system disease.”
Separating Fact From Fiction
Cinema dramatizations often feature a single hospital or doctor who receives a viable lung in the nick of time. Before the rolling credits, a groggy patient thanks the omnipotent surgeon. We leave the show feeling that is the end of the story.

In reality, doctors exhaust all alternative treatments. A spirometer is the main piece of equipment used for basic Pulmonary Function Tests (PFTs). Doctors rule out lung diseases such as asthma, bronchitis, and emphysema with this tests. Many other tests that assure the best possible match include:
- Blood typing – The recipient’s blood type must match the donor’s. This is due to antigens that are present in donated lungs. A mismatch of blood type can lead to a strong response by the immune system and subsequent rejection of transplanted organs
- Tissue typing — Ideally, the lung tissue would also match as closely as possible between the donor and the recipient, but the desire to find a highly compatible donor organ must be balanced against the patient's immediacy of need
- Chest X-ray – PA & LAT, to verify the size of the lungs and the chest cavity
- Pulmonary function tests
- CT Scan (High Resolution Thoracic & Abdominal)
- Bone mineral density scan
- Gated cardiac blood pool scan (MUGA)
- Cardiac stress test (Dobutamine/Thallium scan)
- Ventilation/perfusion (V/Q) scan
- Electrocardiogram
- Cardiac catheterization
- Echocardiogram
A stable patient who is not confined to a hospital receives a pager. Within a moment’s notice, this individual must be willing to relocate to a hospital qualified to perform the surgery and provide follow-up rehabilitation. Automobile driving and many other tasks are suspended for at least 3 months until receiving occupational therapist clearance.
Post-Surgery Recovery
Immediately following surgery, the patient is in an intensive care unit for monitoring, normally for a few days. A ventilator assists breathing. Nutritional needs are generally met with feeding tubes while chest tubes drain excess fluids.
⚠️ Cutaneous complications common post-transplant
As use of lung transplant becomes more common, pulmonologists should be aware of post-transplant dermatologic complications. The most common are HSV-1, HSV-2, varicella zoster, HHV-6, and KSHV. Zoster (shingles) rates in transplant recipients are between 3 and 25 percent and are more common in older recipients of thoracic transplants receiving mycophenolate-containing immunosuppressive regimens. —Cleveland Clinic
Even with full recovery and a daily cocktail of immunosuppressive drugs and antibiotics, the average donor lung longevity is 3 to 5 years. Effectively living without an immune system is challenging. Nerve damage can interfere with common autonomic functions such as coughing. Heart rate responds less quickly to physical exertion. The voice may change.
Survival Prognosis
| 1 year | 5 years | 10 years | |
|---|---|---|---|
| Lung transplant | 83.6% | 53.4% | 28.4% |
| Heart-lung transplant | 73.8% | 46.5% | 28.3% |
A lung transplant can be expensive before, during, and after the surgery. The typical cost is $500,000–$800,000, depending on whether the procedure involves one or both lungs. Health insurance may cover many, but not all, of the costs. Protecting your lungs by avoiding cigarettes, vaping, and wearing masks during annual flu season and especially through a pulmonary pandemic is the course of wisdom to remain healthy.
Enjoy more articles about pulmonology here, or explore ClinicalInsights or ClinicalNovellas.
ClinicalPosters offers human anatomy charts, scientific posters, and other services that compliment articles about pulmonology. Slide extra posters into DeuPair Frames without removing from the wall.
Show your support by leaving an encouraging comment to keep the research going.
Support the writing of useful articles about pulmonology by exploring human anatomy charts, scientific posters, and other products online. You may sponsor specific articles.
ClinicalPosters provides human anatomy charts, scientific posters, and other products that compliment useful articles about pulmonology.
ClinicalPosters offers human anatomy charts, scientific posters, and other products online.
You can sponsor useful articles about pulmonology or donate to further research. Visible content is optimized for device size.