Accurate diagnosis can depend upon the equipment used.
Similar Results At Wildly Different Cost
Unable to interpret the results themselves, for some physicians, an MRI is a figurative black hole into which a patient may be inserted to see what comes out. This often occurs without a definitive diagnosis. The hope is that the radiologist, or more importantly, the examiner of the images, will rule out major illnesses. However, using the wrong equipment can lead to inaccurate and costly conclusions.
Sometimes the terms CT and MRI are used interchangeably. What’s the difference between a CT scan and an MRI? Each machine may resemble a donut hole that encircles a patent. But which is better suited for locating cancers within the body?
This can depend upon where tumors may be located. Multiple Myeloma, for example is a bone cancer that shows up better in a CT (or CAT) scan since, much like a high-resolution x‑ray, it is best suited for bone injuries, lung or chest imaging, and detecting cancers. CT scans are widely used in emergency rooms because the procedure takes less than 5 minutes.
An MRI, on the other hand, can take up to 30 minutes. It excels in distinguishing soft tissues (i.e. ligament and tendon injury, spinal cord injury, brain tumors etc.). One advantage of an MRI is that it does not use radiation, while CT scans do. This radiation is harmful if there is repeated exposure, so MRIs may be used to evaluate progress during a course of cancer treatment.
A PET scan uses nuclear medicine imaging to produce a three-dimensional 3D picture of functional processes in the body. PET scans provide metabolic information and are increasingly read alongside CT or MRI (magnetic resonance imaging) scans, which provide anatomic information.
Patient out-of-pocket costs vary considerably depending upon health plans. Pricing has declined dramatically over the years. Emergency room rates differ from hospital or outpatient prices. Insurance companies generally do not pay maximums. View monetary values merely as relative comparisons between various technologies.
Radiology Comparison Chart
MRI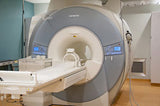
|
CT (CAT) Scan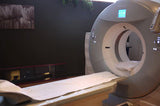
|
PET Scan
|
|
|---|---|---|---|
| Cost | MRI costs range from $1200 to $4000 (with contrast); which is usually more than CT scans and X-rays, and most examining methods. | CT scan costs range from $1,200 to $3,200; they usually cost less than MRIs (about half the price of MRI). | PET scans cost $3,000 to $6,000; much higher than regular CT scans. |
| Update | Outdated prices are for relative comparison only. An MRI can now be obtained for $300 to $800. | ||
| Time taken for complete scan | Scanning typically runs about 30 minutes. | Usually completed within 5 minutes. Actual scan time is usually less than 30 seconds. Therefore, CT is less sensitive to patient movement than MRI. | Usually takes 2 to 4 hours. |
| Radiation exposure | No radiation. MRI machine control/ |
The effective radiation dose from CT ranges from 2 to 10 mSv, which is about the same as the average person receives from background radiation in 3 to 5 years. Usually, CT is not recommended for pregnant women or children unless absolutely necessary. | Moderate to high radiation. |
| Effects on the body | No biological hazards have been reported with the use of the MRI. | Despite being small, CT can pose the risk of irradiation. Painless, noninvasive. | Radiation risk from the injection of a radioactive tracer is about the same as an X-ray. |
| Scope of application | MRI is more versatile than the X-ray and is used to examine a large variety of medical conditions. | CT can outline bone inside the body very accurately. | PET scans can image biological processes within the body. |
| Acronym for | Magnetic Resonance Imaging | Computed (Axial) Tomography | Positron Emission Tomography |
| History | First commercial MRI in 1981, with significant increase in MRI resolution and choice of imaging sequences over time. | The first commercially viable CT scanner was invented by Sir Godfrey Hounsfield in Hayes, United Kingdom; the first patient brain-scan was done on 1 October 1971. | The compound was first administered to two normal human volunteers by Abass Alavi in August 1976 at the University of Pennsylvania. |
| Principle used for imaging | Body tissue that contains hydrogen atoms (e.g., in water) is made to emit a radio signal, which is detected by the scanner. Search for "magnetic resonance" for physics details. | Uses X-rays for imaging | Radioactive tracers that emit positrons are used. The positrons are tracked by the system to generate a 3D image over time. |
| Limitation for Scanning patients | Patients with cardiac pacemakers, tattoos, and metal implants are contraindicated due to possible injury to the patient or image distortion (artifact). Patients over 350 lb may be over the table weight limit. Any ferromagnetic object may cause trauma/ |
Patients with any metal implants can get CT scan. A person who is very large (e.g. over 450 lb) may not fit into the opening of a conventional CT scanner or may be over the weight limit for the moving table. | Patients with any metal implants can get CT scan. A person who is very large (e.g. over 450 lb) may not fit into the opening of a conventional CT scanner or may be over the weight limit for the moving table. |
| Intravenous contrast agent | Very rare allergic reaction. Risk of nephrogenic systemic fibrosis with free Gadolinium in the blood and severe renal failure. It is contraindicated in patients with GFR under 60 and especially under 30 ml/min. | Non-ionic iodinated agent covalently binds with fewer side effects. Allergic reaction is rare but more common than MRI contrast. Risk of contrast-induced nephropathy (especially in renal insufficiency [GFR<60], diabetes and dehydration). | Non-ionic iodinated agent covalently binds with fewer side effects. Allergic reaction is rare but more common than MRI contrast. Risk of contrast-induced nephropathy (especially in renal insufficiency [GFR<60], diabetes and dehydration). |
Not all equipment is created equally. CT scanners range from 4‑slice to 16- or 64‑slice units. MRI machines are available in 1.5‑T (Tesla) and 3‑T with higher image quality and shorter scanning times. An experienced oncologist is more likely to be familiar with and have access to better equipment. A diagnosing factor that is equally as important as the equipment is the skill of the one interpreting the images. For critical decisions, a second radiologist reading may be warranted.
How Accurate Is An MRI Report?
True or false? A false negative is when a test reveals favorable news that contradicts empirical evidence. Conversely, a false positive occurs when an incorrect unfavorable condition is reported. One might assume that results from a million-dollar piece of equipment would represent an authoritative conclusion.
Quality of the imaging coils put around the body part being scanned, and the computer programs used to control the imaging and analyze the images, are important. But perfectly tuned equipment is only as reliable as the person who views the images and prepares the reports.
Statistics From Clinical Studies
Radiologist Emmanuelle Bouic Pagès, MD, and colleagues at CHU Lapeyronie, Montpellier, France, reported in the magazine Radiology that potential observer error existed in 47% of breast MRI studies performed from January 2005 to December 2010. Medscape clarifies that the many critics who came to the defense of the equipment may not have paid attention to the report’s content.
“Machines don’t make diagnoses; people do,” Herbert Y. Kressel, MD, editor of Radiology, explained to Medscape. “This is a study about errors made by people using the results of MRI exams.” Misinterpretation produced most of the false-positive results, according to the study. [1] With false-positive readings, a patient may undergo an unnecessary mastectomy or amputation.
It is hoped that the error rate will be much lower wherever we might have tests performed. To determine if better resolution (higher Tesla) improves evaluation, a study by Grossman JW, et al compared accuracy rates of 3-T and 1.5-T MRI in diagnosing medial and lateral meniscal tears in 200 patients. Fifteen of the 26 missed meniscal tears were not seen in retrospect, even with knowledge of the tear type and location. The study concluded comparable accuracy of 3-T and 1.5-T MRI. [2]
A study by Akiko Shimauchi, et al of 220 sequentially diagnosed breast cancer lesions found seven (3.2%) false negative results—considerably fewer than other published studies. Although the overall sensitivity of cancer detection was high (96.8%), it should be emphasized that a negative MRI should not influence the management of a lesion that appears to be of concern on physical examination or seen by other imaging methods. [3]
A negative MRI should not influence the care of a lesion.
Living up to his name, an orthopedic surgeon who blogs under the nom de plume Angry Othopod vents:
“Did you know that a growing number of doctors don’t even read the tests themselves? MRI is unnecessarily overused. In a study of 221 patients who had MRIs, the results showed that only 5.9% actually needed to have an MRI done.… If you suspect your doctor is just being quick or using MRI to reach that ‘aha’ moment, then you’re in a bad scenario.”
“When I order an MRI, I am 90% certain about what the results are going to show. Doctors need to have a clear-cut idea of what they can expect to see from the results. Next time you’re told to get an MRI, and your doctor has little clue to your diagnosis, you may want to get a second opinion. Also, be sure to ask the physician if they read the MRI themselves.” [4]
Unless it is of considerable volume, a mass detected on an X-ray, MRI, or CT scan is often a dot or speck requiring a judgment call. Determining whether a dot is an anomaly depends upon the skill, experience, and alertness of the technician. Add these variables to the need for properly tuned equipment, and you can see there is a margin for error.
“Advances in AI algorithms have narrowed the gap between computers and human experts in detecting breast cancer in digital mammograms,” Ioannis Sechopoulos, PhD, of Radboud University Medical Centre in Nijmegen, the Netherlands, and colleagues wrote. [5] If a radiologist reports back with positive results, get a second opinion. When results are negative, a second opinion is still advised.





 Romance & Health Intertwine. Fall in love with a captivating romance miniseries that explores the essence of well-being. Become a ClinicalNovellas member for heartwarming tales.
Romance & Health Intertwine. Fall in love with a captivating romance miniseries that explores the essence of well-being. Become a ClinicalNovellas member for heartwarming tales.





