Circulation problems overlap patient groups.
Diabetic Foot Disorders Are More Common
Diabetes can be a precursor to peripheral artery disease (PAD) but the disease can also become manifest without prior history of diabetes. Many PAD patients are symptomless until advanced stages.
Untreated PAD can be dangerous because it may lead to painful symptoms or loss of a leg. PAD patients have an increased risk of coronary artery disease, stroke and myocardial infarction (heart attack).
PAD is the constriction of arteries in the lower extremities. According to the National Heart, Lung and Blood Institute (NIH), people with PAD may have symptoms of cramping in the affected leg(s) when walking or climbing stairs, pain, numbness, aching, or heaviness in the leg muscles.
The discomfort results because the increased blood flow required during physical activity is restricted. Rest lessens blood flow, thereby relieving the discomfort. This contrast is called intermittent claudication. Other signs and symptoms of PAD include:
- Weak or absent pulses in the legs or feet
- Poor nail growth on the toes and decreased hair growth on the legs
- Erectile dysfunction (especially among men who have diabetes)
Those with diabetes might confuse PAD pain with a neuropathy, a common diabetic symptom that is a burning or painful discomfort of the feet or thighs. In most cases, lifestyle changes, exercise and claudication medications are enough to slow the progression or even reverse the symptoms of PAD. According to the American Heart Association, symptoms of severe PAD include:
- Leg pain that does not go away after excersize stops
- Sores or wounds on the toes, feet or legs that heal slowly, poorly or not at all
- Gangrene
- Lower temperature in one leg or foot compared to the other leg or to the rest of your body
An inexpensive painless test that takes only a few minutes is called Ankle-Brachial Index (ABI). It compares the blood pressure in feet to the blood pressure in arms to determine how well blood is flowing. Normally, the ankle pressure is at least 90 percent of the arm pressure, but with severe narrowing it may be less than 50 percent.
This test may be performed in conjunction with a peripheral vascular examination (PVS). If an ABI reveals an abnormal ratio between the blood pressure of the ankle and arm, more testing may be required.
My Introduction to PAD
Years ago I found myself in the unanticipated position of medical liaison for an advanced-stage PAD patient—a relative. She had developed gangrene in a toe that physicians had been treating for a couple of months.
A thousand questions swarmed through my mind: How did she develop gangrene without being exposed to cold? Why are doctors allowing it to fester? What is the immediate course of treatment? How come I was brought in at such a late stage of the disease progression?
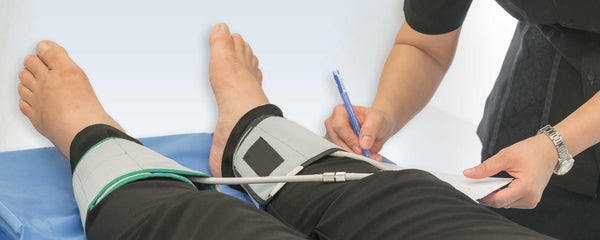
Leg pulse measurement during vascular examination.
The lack of circulation in lower extremities can lead to foot ulcerations. This can resemble the more common diabetic foot ulcer. We scheduled an appointment to see her neurology specialist and assess neuropathy. He scheduled a peripheral angiogram. Her toe continued to fester as we waited weeks for the results.
At the next appointment we were shown radiopaque x-rays and told that the three tibial arteries were extremely narrowed. Neither was a candidate for a stent or bypass. Such severe circulation would affect healing after localized amputation. The medical recommendation was amputation of at least the lower leg.

Right foot healed with amputated toes.
I began to see why there was treatment hesitation. My relative argued to remove just her gangrenous toe. She was locking horns with the physician and wanted to find someone that would appease her demands. Eventually a surgeon stepped up. However, healing issues anticipated by prior professionals surfaced. Continuing to fight extensive amputation, the surgeon agreed to remove half the foot. Surprisingly, the amputation healed with her poor circulation.
Southern Extremities
From here, things went south. Post-surgical rehabilitation is arguably more important than the surgery itself. Though admitted to a private room in a beautiful facility overlooking a flower garden, my relative became uncooperative. She wanted to go home.
Unable to keep her against her will, she was discharged under the care of three assistants—a nurse to administer medications and provide physical therapy, someone to drive her to and from medical appointments, and someone to help with household chores—the trifecta of optimum homecare.
But remember I said things went south. The paranoia resulting in her early rehab discharge led her to dismiss all the assistants! Living 50 miles away from me, this presented a new challenge.
We turned to a homecare agency that was able to send one nurse. She too was summarily dismissed. After three weeks, no homecare agency would accept the assignment. Eventually, an independent homecare provider able to put up with stubbornness stepped in.
Despite best efforts, rehabilitation was nonexistent. My relative cherry picked medications, ate a minimal amount of food and refused to exercise. When my brother who had ambitious plans for her relocation across the country asked for a prognosis, I said she had about 30 days more. The accuracy of that statement was sobering. A month later we held her memorial service.
The death certificate listed cause of death as pulmonary embolism resulting from “diabetes mellitus.” (There was no mention of PAD. She had never been prescribed diabetes medication.) Recall, I was with her during the neurological diagnosis.
From April to October 4, 2005, I saw firsthand how PAD coupled with disregard for medical treatment led to a relative’s demise. Do not let the chair you are sitting in exacerbate circulation problems. Take steps to prevent and treat peripheral artery disease before it turns deadly.
Enjoy more articles about cardiology here, or explore ClinicalInsights or ClinicalNovellas.
ClinicalPosters offers human anatomy charts, scientific posters, and other services that compliment articles about cardiology. Slide extra posters into DeuPair Frames without removing from the wall.
Show your support by leaving an encouraging comment to keep the research going.
Support the writing of useful articles about cardiology by exploring human anatomy charts, scientific posters, and other products online. You may sponsor specific articles.
ClinicalPosters provides human anatomy charts, scientific posters, and other products that compliment useful articles about cardiology.
ClinicalPosters offers human anatomy charts, scientific posters, and other products online.
You can sponsor useful articles about cardiology or donate to further research.






 Romance & Health Intertwine. Fall in love with a captivating romance miniseries that explores the essence of well-being. Become a ClinicalNovellas member for heartwarming tales.
Romance & Health Intertwine. Fall in love with a captivating romance miniseries that explores the essence of well-being. Become a ClinicalNovellas member for heartwarming tales.






