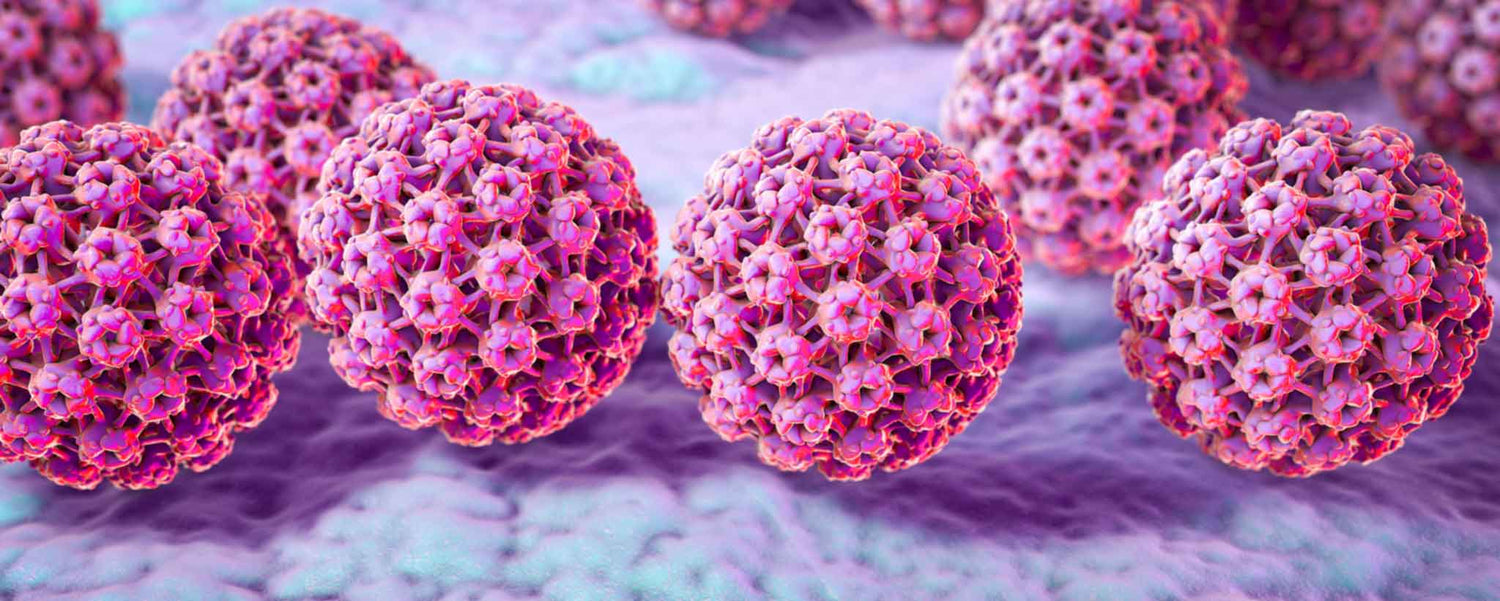
The virus that causes oral cancer shares characteristics with cervical cancer.
⚠️ Use Discretion: Graphic human anatomy.
Body Invaders
Imagine single-handedly battling over 120 soldiers. Four are special ops. They intend to literally get under your skin—a goal already achieved in more than three-quarters of their targets. The prominent human papillomavirus soldiers go by the names HPV-16, HPV-18, HPV-31, and HPV-45. They invade the skin with nearly invisible and often flat cancer-causing growths. [1]
The Attack
The most dangerous attackers, HPV-16 and HPV-18, thrive in the genital tract and oral mucosa, such as the back of the tongue, the oropharynx, the tonsils, and the tonsillar pillars; they are responsible for 70 percent of cervical cancers.
HPV-6 and HPV-11 frequently appear as raised non-cancerous warts on the arms, legs, and other skin areas. [1] The most common types are HPV-1, 2, and 4, which cause warts on the hands (palmar warts) and feet (plantar warts). [2]
Bowen’s disease is generally indicated by HPV-31, 54, 58, 61, 62, and 73. [3] HPV-6 and 11 may suggest benign recurrent tumors of laryngeal and respiratory papillomatosis [4,5] and cauliflower-like genital warts, [2] called condylomata.
HPV stands for human papillomavirus. Common causes of this vast series of viruses are smoking, chewing tobacco, immoderate alcohol consumption, and promiscuous sex. In fact, over 30 types of HPV can be passed from one person to another through sexual contact. [6]
Strains of HPV can also be transferred from seemingly “safe” contact, like open-mouth kissing or even skin-to-skin contact [6] with an infected individual—touching an exposed wart. Nearly everyone has some type of HPV at some point in their life, and chances increase with age.
Some types of HPV are innocuous; others are automatically eliminated by a healthy immune system. Most HPV infections in young females are temporary and have little long-term significance. Seventy percent of infections are gone in 1 year and 90 percent in 2 years.
Over 30 types of HPV can be passed… through sexual contact.
But when the infection persists—in 5 to 10 percent of infected women—there is a high risk of developing cervical precancer (lesions on the cervix), which can progress to invasive cervical cancer. This process usually takes 15–20 years, providing many opportunities for detection and treatment of the pre-cancerous condition, often with high cure rates. [7]
HPV From Fellatio & Cunnilingus Risks

When aroused, the vaginal cavity is lubricated by a combination of plasma and mucus—neither of which is considered edible bodily fluids.
For those considering oral sex as a form of contraception, there is a remote possibility that accidental vaginal exposure to semen without copulation may result in pregnancy. While upwards of half a million spermatozoa are released per ejaculation, it only takes one to fertilize a female egg. [8]
For most people, a more serious deterrent is the spread of sexually transmitted infections (STIs). Long gone is the simple solution of taking penicillin to get rid of a venereal disease. Syphilis is seeing a resurgence in Europe, Germany, France, the Netherlands, Amsterdam, and the U.S. [9]
There are now many STIs resistant to penicillin. Chlamydia, human papillomavirus (HPV), gonorrhea, herpes, hepatitis (multiple strains), and other sexually transmitted infections—can be transmitted through oral sex. [10] Many things are concealed under the cover of darkness. Look before you lick.
Physical cleanliness is important. But despite good hygiene, there are plenty of potential gynecological disorders that could be lurking down there. Some result from multiple (infected) sex partners, while infections can occur in someone who is not sexually active. In addition to normal acidic microflora, the vagina can be a breeding ground for everything from abnormal bleeding and yeast infection to HPV and AIDS.
Hematospermia is the presence of blood in semen. It is most often a benign and idiopathic symptom, but can sometimes result from medical problems such as a urethral stricture, infection of the prostate, or a congenital bleeding disorder. [11] Bloody semen can unknowingly be ejaculated during fellatio. STIs can be transferred via an open canker sore or infected semen.
Something more insidious may cause one to pause when contemplating oral sex.
Men and women can suffer bouts with intertrigo (or jock itch) in the groin, anus, and beneath the breasts. Intertrigo is a rash in the creases of overlapping skin associated with sweating, skin-on-skin friction, and occlusive clothing. Intimate contact with objects that harbor fungus spores (e.g., unwashed towels, bedding, or hair combs, moldy tile grout) can cause intertrigo since the fungus can thrive on dead skin cells for a long time.
People taking broad-spectrum antibiotics or those with diabetes are at risk of developing the rash. [12] Thoroughly pat dry after showering or bathing and apply talcum powder (or antifungal powder if a rash is present) to folds of skin to control jock itch. Even with these precautions, something more insidious may cause one to pause when contemplating oral sex—throat cancer.
Prevent the Attack
The best defense against dangerous types of HPV is prevention. Two FDA-approved HPV vaccines show greater efficacy before infection for females between 9 and 26 years old (Gardasil and Cervarix). [13] About 30 percent of cervical cancers are unpreventable with these vaccines.
Avoid risky sex and non-monogamous practices. Sexually active women should have regular Papanicolaou (Pap) smears to detect early signs of cervical cancer. The CDC recommendation is that all children aged 11 or 12 years old should get two shots of the HPV vaccine six to twelve months apart. [14]
One person per hour dies from oral cancer. Have six-month dental examinations performed by a professional who screens for oral cancer. Many dentists are using fluorescence devices such as the VELscope to discover basal cell carcinoma a year or more before it becomes visible to the naked eye. Upon discovery, they are likely to refer patients to an otolaryngologist (ENT doctor).
The American Academy of Dermatology recommends annual examinations for lumps and moles. A dermatologist should examine new moles appearing after age 20. [15] Death rates from cervical cancer have halved over the past 30 years, reflecting better treatment. [16,17] Though outnumbered, you can successfully battle HPV and reduce the incidence of cervical and oral cancer with defensive action.
Enjoy more articles about women here, or explore ClinicalInsights or ClinicalNovellas.
ClinicalPosters offers human anatomy charts, scientific posters, and other services that compliment articles about women. Slide extra posters into DeuPair Frames without removing from the wall.
Show your support by leaving an encouraging comment to keep the research going.
Support the writing of useful articles about women by exploring human anatomy charts, scientific posters, and other products online. You may sponsor specific articles.
ClinicalPosters provides human anatomy charts, scientific posters, and other products that compliment useful articles about women.
ClinicalPosters offers human anatomy charts, scientific posters, and other products online.
You can sponsor scholarly articles about women or donate to further research. Some content may be inappropriate for younger audiences. Visible content is optimized for device size.






 Romance & Health Intertwine. Fall in love with a captivating romance miniseries that explores the essence of well-being. Become a ClinicalNovellas member for heartwarming tales.
Romance & Health Intertwine. Fall in love with a captivating romance miniseries that explores the essence of well-being. Become a ClinicalNovellas member for heartwarming tales.




