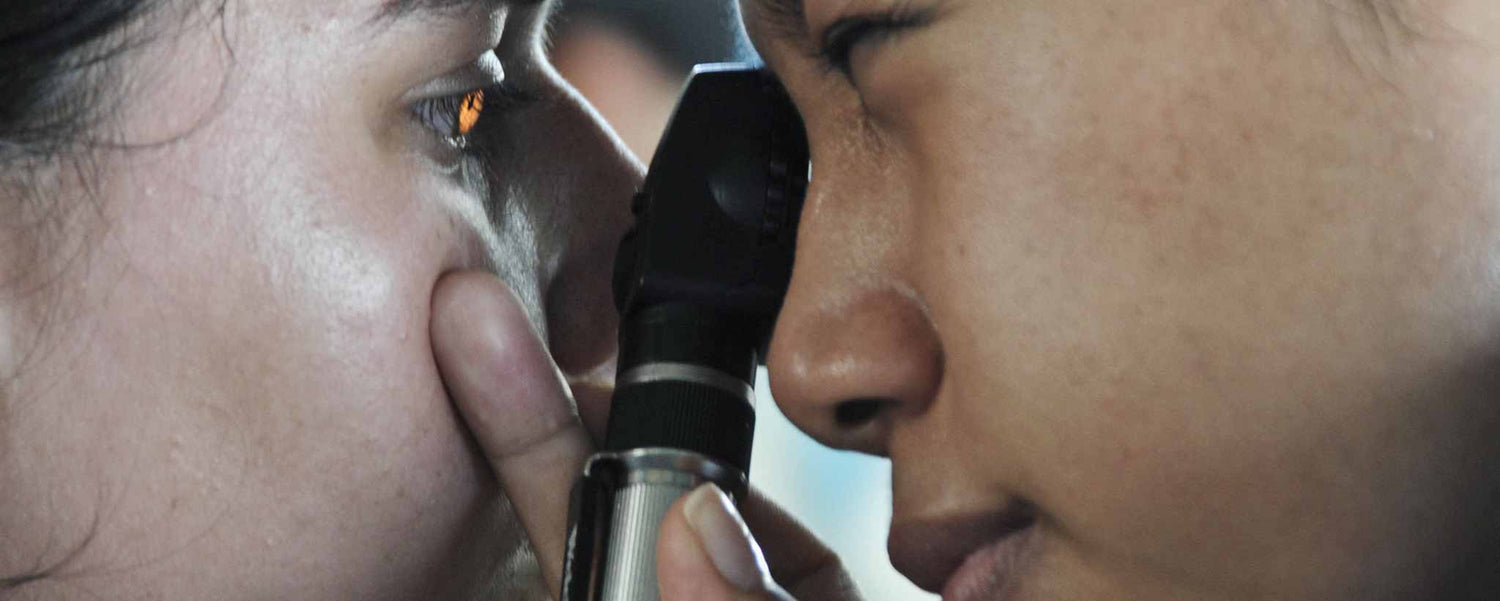Sometimes, what looks like a floater is actually an eyelash or eyebrow hair hanging within your field of view. What if something is within your eye?
Visual Distractions
Do you see spiders floating around the room? If you say that out loud when they are absent, people might think you are losing your mind. However, there can be an ophthalmological reason for this phenomenon.
With better functioning in youth, the eyes are remarkable focusing mechanisms. Over time, muscles that aid in focusing weaken. Corrective lenses have become common. But eyes remain sensitive to abnormal interference. Mild floaters are normal and may resolve on their own.
To prevent floaters, try to keep your fingers from your eyes, particularly when sleeping. You can wear a sleep mask if necessary. Do not rub them too vigorously. Avoid contact sports that can damage the eyes.
There is a cause for concern if you notice a sudden increase in the number of floaters, if part of your vision appears blocked by a dark curtain, or if you observe disturbing flashes of light. In such cases, contact your doctor immediately to save your vision.

Simulation of floaters within the left eye while looking at the sky: Floaters may resemble black or gray blobs, specks, strings, spiderwebs, or cobwebs that drift about when you move your eyes and appear to dart away when you try to look at them directly. Ambient light can either diminish or accentuate appearance.
Sometimes, what you assume is a floater may be an eyelash or eyebrow hair hanging in your field of view. Removal of the lash rectifies the problem. If there is no irritation but something keeps blocking your sight, blink several times while looking straight ahead.
If it moves, it could be other debris—perhaps mucus—on the surface. If it remains in the same relative position, though seeming to dart back and forth as you look from side to side, the cause is likely one or more internal floaters.

Floaters can range in appearance from dots that are barely noticeable to what might seem like insects or cobwebs constantly hovering in front of your eye. White or light backgrounds make them most apparent. If they interfere with focus or reading, express your concerns to an ophthalmologist or optometrist.
During the exam, they may dilate your eyes with drops, making it possible for the doctor to look inside. Various machines can create images of your eye interior without dilation.
An optometrist or ophthalmologist wants to rule out retinal detachment, macular degeneration, or glaucoma. With age or trauma, the translucent vitreous membrane can begin separating from the retina. This process, called posterior vitreous detachment (PVD), can take 3 months or longer. It may get worse, in terms of distracting floaters, before it gets better.
A follow-up exam is usually required in 6–8 weeks unless there are more severe signs of retinal detachment, which have similar symptoms. Eventually, gravity should pull the membrane down out of view. The membrane may also dissolve over time.
Retinal detachments are usually painless and are not associated with headaches. There are very rare causes of retinal detachment associated with systemic diseases, such as hypertension, that may have associated headaches.
Transient diminished vision in one eye with migraines is generally unrelated to floaters. It may be a condition known as retinal migraine. This has constricting blood vessels as its cause. It may be hereditary. If frequent, treatment is the same as for other migraines.
For excessive floaters that interfere with daily activities, an operation called a vitrectomy is possible. In this procedure, the entire vitreous gel contents of an eye is replaced with saline.
Alternatively, a few doctors have the skill and equipment to target specific floaters with laser vitreolysis. There is a chance that the laser may disperse larger floaters into smaller ones rather than vaporize them. Floaters that are too close to the crystalline lens or retina can be problematic. In cases where dozens of small floaters are visible, a laser may not be the best option.
Differential
Retinal detachment is a disorder of the eye in which the retina separates or breaks from the layer underneath. Symptoms include an increase in the number of floaters, flashes of light, and worsening of the outer part of the visual field.
Macular degeneration, also known as age-related macular degeneration (AMD or ARMD), is a medical condition that may result in blurred or no vision in the center of the visual field. There is no cure, but dietary supplements may slow progression in those who already have the disease.
It is thought that most cases of glaucoma (although not all) are caused or enabled by an increase in intraocular pressure. Pressure increases either when too much aqueous humor fluid is produced or by decreased aqueous humor outflow.
The D-Eye Retina macro-lens adapter (ophthalmoscope) for iPhone allows eyecare professionals to photograph or make videos of the inner eye. Within seconds, an ophthalmologist can diagnose a range of eye disorders without dilating pupils.
As you can see, vision care professionals do more than prescribe and fit eyewear. When getting eye exams, speak up about issues that concern you, even if extra tests may cost more. What will you do about chronic floaters? In most cases, nothing. For patients who undergo vitrectomy, the road to recovery is several months. Discuss options with your eye doctor.
Enjoy more articles about vision here, or explore ClinicalInsights or ClinicalNovellas.
ClinicalPosters offers human anatomy charts, scientific posters, and other services that compliment articles about vision. Slide extra posters into DeuPair Frames without removing from the wall.
Show your support by leaving an encouraging comment to keep the research going.
Support the writing of useful articles about vision by exploring human anatomy charts, scientific posters, and other products online. You may sponsor specific articles.
ClinicalPosters provides human anatomy charts, scientific posters, and other products that compliment useful articles about vision.
ClinicalPosters offers human anatomy charts, scientific posters, and other products online.
You can sponsor useful articles about vision or donate to further research. Visible content is optimized for device size.