⚠️ Reader Discretion. Graphic images.
Two Words No Patient Should Hear
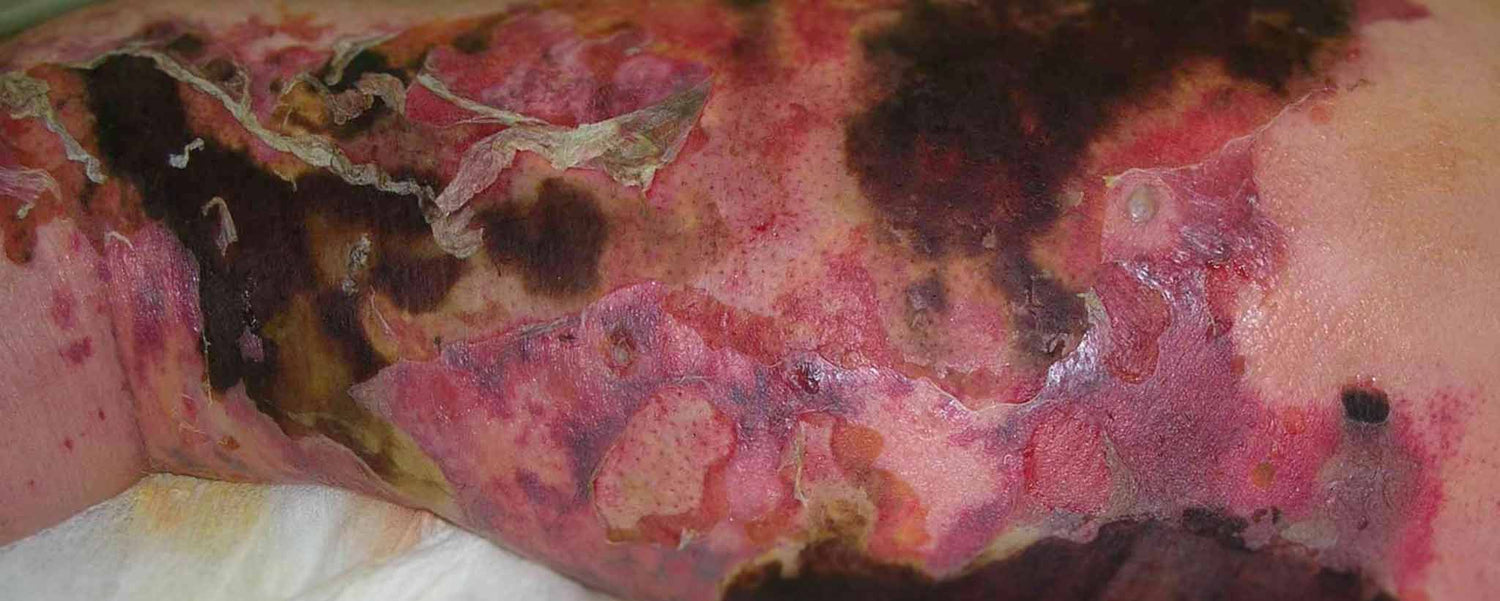
Necrotizing fasciitis. Take care of your skin, or you could lose much of it—along with muscles and tendons. Clean and apply antibacterial ointment like Neosporin to minor cuts. Have a doctor treat more serious wounds and 2nd-degree burns. A broken skin barrier can lead to serious infection. Affecting about 0.4 people per 100,000 per year in the U.S., necrotizing fasciitis is a rare bacterial infection that quickly spreads.
Necrotizing means causing the death of tissues. Fasciitis means inflammation of the fascia (the tissue under the skin that surrounds muscles, nerves, fat, and blood vessels). The condition is sometimes called flesh-eating disease. Rarely contagious, the bacteria most commonly enter the body through a break in the skin, including:
- Cuts and scrapes
- Burns
- Insect bites
- Puncture wounds (including IV drug use)
- Surgical wounds

How People Get Necrotizing Fasciitis
Highly infectious necrotizing fasciitis can form after an injury that does not break the skin (blunt trauma). Even though minor illnesses can cause such symptoms, people should not delay getting medical care. See a doctor right away if you have these symptoms after an injury or surgery.
Late-stage symptoms of necrotizing fasciitis can include:
- Ulcers, blisters, or black spots
- Changes in skin color
- Pus/oozing from an infected area
- Dizziness
- Fatigue (tiredness)
- Diarrhea or nausea
Since necrotizing fasciitis can spread rapidly, patients often must get surgery very quickly. Doctors also give antibiotics through a needle into a vein (IV antibiotics) to try to stop the infection.

Open wound after debridement. Image by Morphx1982 licensed under the Creative Commons license.
Sometimes antibiotics cannot reach all of the infected areas because the bacteria have killed too much tissue and reduced blood flow. When this happens, doctors have to surgically remove the dead tissue in a procedure called debridement. It is not unusual for someone with necrotizing fasciitis to end up needing multiple surgeries or amputations.